A Sleepy, Little Cancer Cell
New Ways to Detect Early Spread of the Cancer
“It is not good to wake a sleeping lion.” – Sir Philip Sidney
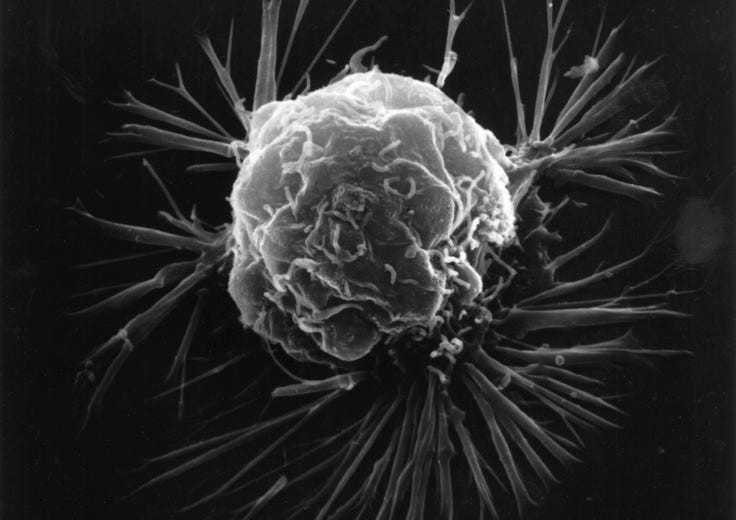
I was sitting in the second row of the auditorium and studying a projected image of the bone marrow. The cells looked like they had been painted with vibrant colors, but in this case the paint was the result of fluorescent antibodies that were binding to different cell types. The speaker was pointing out a single green cell in the middle of the image in a sea of yellow and pink.
A sleepy, little cancer cell.
It was sleeping for now, but at some point, it might wake up angry and begin dividing. Once it started, it wouldn’t stop dividing. And then it would decide to take a vacation to places far away, like the lungs or the bone or the brain.
When this little cell and its friends had reached a critical point in their wild party dedicated to making more of themselves, they would cause a problem for the patient. The patient would report a symptom to their doctor. A scan would be ordered. And the metastasis would be discovered.
The scientist speaking at the front of the room was trying to discover why this single sleepy little cancer cell would suddenly wake up to begin the process of metastasizing long after the patient had finished their chemotherapy course. The scientist was a hero to me.
Because nothing terrified me more than the idea of this little green cell.
Within the month, my husband would take the last pill of his oral chemotherapy, a drug to stop breast cancer cells from dividing called a CD4/6 inhibitor. It was a newer drug used specifically to treat hormone receptor-positive breast cancers, which was the first breakthrough in a very long time to improve patients’ survival.
When he started the drug, he had finished a whole year of treatments beginning with a mastectomy and followed by traditional chemotherapy and radiation. The CD4/6 inhibitor was originally being used only to treat metastatic or advanced breast cancers like his. Now, it was being offered to patients with early breast cancers that had features suggesting a high-risk of recurrence.
His oncologist said that he could only stay on the CD4/6 inhibitor for two years. She didn’t have to explain why he would only stay on the drug for this period. I had already looked it up.
Cancers often became resistant to the CD4/6 inhibitor over time. About 1 in 5 breast cancer patients that were treated would never respond to the drug because their cells had already acquired small changes in their DNA to allow them to keep dividing. Some patients would respond initially but then the cancer would come back when the cells had become resistant.
After two years, the drug should have already done its job to kill any remaining breast cancer cells that the chemotherapy and radiation hadn’t eliminated. If it hadn’t, any remaining breast cancer cells would eventually acquire resistance to the drug and come back anyway. Staying on the drug forever wasn’t a good idea.
A breast cancer cell.
It was not a certainty that he had dormant breast cancer cells in his bone marrow. But I thought it was highly likely given the extent of his disease before treatment began. Even more likely knowing that an estimated 40% of breast cancer patients have cancer cells that have already spread to the bone marrow at the time of their diagnosis. Here, they would lie in wait until some undetermined time in the future. Then, they would wake up and start dividing.
I wanted so badly for my husband to stay on a drug to prevent this from happening. Preferably, he would take the drug forever to remind those sleepy, little cancer cells in the bone marrow that they needed to behave.
Stay asleep! Leave him alone, I would think. The girls are only in 7th and 9th grade. They need their father and I need my husband.
The scientist at the front of the room was talking about how the neighboring cells and environment around the sleeping cancer cell were important in determining whether it stayed asleep or woke up to start dividing.
“Why don’t we see cancers spread to muscle?” he asked the room full of PhD graduate students and scientists.
Good question. It almost never happened. Cancers would spread to the lungs, the liver, the bones, the brain, and the intestines. But the muscle? It’s rare.
“It’s the neighborhood,” he said. “The signals sent by nearby cells and their environment determine whether the cancer cell will wake up, spread to another part of the body and take hold.”
My husband’s oncologist told us about a cancer trial performing bone marrow biopsies in patients like him to look for dormant breast cancer cells. If cancer cells were found in his bone marrow, the trial would offer him some sort of treatment. But he wouldn’t be eligible for this trial for another 6 months to a year after he had stopped the CD4/6 inhibitor. Presumably, they wanted to wait a while to allow any remaining cancer cells in the bone marrow to multiply and make them easier to detect.
While she had encouraged my husband to enroll in this cancer trial, she hadn’t mentioned the new blood tests available to the public that would look for tumor DNA in a blood test. I had started looking into these tests already as there was no waiting period until my husband would qualify.
The procedure was simple. First, the company would request a piece of the original tumor that had been saved by the pathology department at the time of surgery. Then, they would design a blood test to look specifically for tumor DNA identical to the original tumor.
Very clever and a great use of technology.
Yet, I could understand why his oncologist hadn’t mentioned these tests. If the test was positive, it would trigger anxiety for the patient and expensive testing to find the source of the tumor DNA. Despite the testing, the source might not be found if there were only a few cancer cells producing the tumor DNA.
Where would that leave the doctor and the patient? The wild west. No man’s land. The moon. That is where it would leave them. The risk for a cancer recurrence was higher if tumor DNA was detected, but when it might recur and the best course of action to prevent the recurrence was unknown.
The unsettling image of that little green cell swirled around in my brain. Up, down, upside down. The little green cell stayed in the center of the image with the pink and yellow cells around it becoming a fast-moving blur.
Stay asleep, my little enemy, while we work out what to do next.



Thank you for sharing this. I can’t imagine how you must feel. There are always so many things to consider. And we are beautifully human… Your words touched me in surprising ways.
I read this not long after I had a conversation with one of my daughters, who expressed that every time she hears me cough, it triggers a concern. I should say a fear. All I could think of was to hold her closer. When the cancer came back it was in the lungs. I asked my other two children. They experience something similar. A fear that runs underneath, they can seem to shake off.
The other thing is that I am on the CDK 4/6 protocol. I have been on it for 2 years now. For some reason, my mind went to that place. The clock is ticking. I am almost at the median of the statistics. What if in 8 months, it stops working?
Because right now, it works, but how long can my body take it. I just went through a nasty cold and there is not much fight happening in terms of neutrophil.
I reread your article and I also found hope. The hope of transcendent healing. We are humans. We are not just a bunch of cells or just one… We have the power of our thoughts and of our hearts. Life can be transformed in an instant.
Hope connects us to parts of ourselves that can ignite changes. But can also open us to discoveries and lead us on new paths.
It doesn’t matter how much time is left (we will never know how much anyway) what matters is where we stand right now. In that moment anything is possible.
Kristina, meeting you is the highlight of the new year. I have grown a lot since our first contact. You have opened my mind to new perspectives on how to approach cancer and how it impacts the ones I love.
Continue to share, please.
Scary situation but you wrote about it beautifully